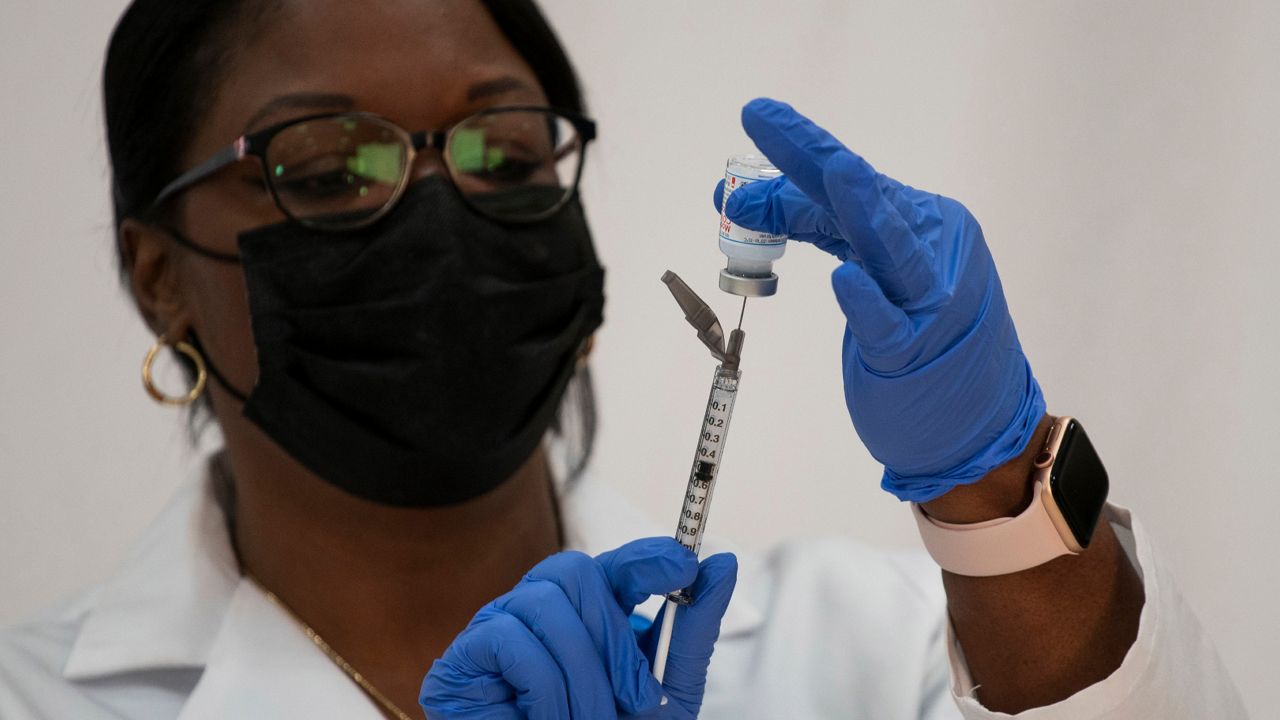
The distribution of the first COVID-19 vaccines has not gone as quickly as planned. Nationally, the goal of 20 million doses by the end of 2020 did not meet the target.
So far, Gov. Andrew Cuomo reported Thursday 430,000 doses have been administered as frontline health care workers and nursing home residents and staff receive the first batch of the vaccinations.
The number of shots each day has been steadily increasing this week, Cuomo said in a conference call with reporters. And more than 6,000 sites ranging from pharmacies to public college campuses, have been identified as sites for mass vaccinations once larger pools of people are eligible.
Essential workers including police officers, firefighters, teachers and people over age 75 will be included in the next round of vaccines. It's not yet clear when they will begin.
Cynthia Leifer, an associate professor of immunology at Cornell University believes there could have been a better roll out of the vaccine's distribution. She also believes the problems can be fixed.
Spectrum News: Walk us through what the issues have been with vaccine distribution in the United States and New York.
Associate Professor Cynthia Leifer: Generally one of the first hurdles that we have to get through is producing enough vaccine to immunize everyone. Part of Warp Speed put money into that. I think the manufacturing is going as fast as we can go.
Once we distribute it, we have to get it out to people. What are the barriers there? I think there are too few distribution sites, especially in New York, but nationwide as well. Right now, the majority of the distribution sites are at hospitals and medical care facilities. I think we can expand that.
I also think another important point is expanding the hours people can get vaccines. A lot of people are working and trying to get to a particular place at a particular time can be difficult The more we can expand those areas I think would be great.
And the third thing is we have a great system for prioritizing who gets the vaccine first. But I think we need to keep in mind the prioritizing doesn’t mean excluding. So we need to make sure that if whoever is first in line isn’t available, that we jump down the line very quickly and we’re not letting those vaccines sit around too long.
SN: Was it mistake initially relying on hospitals for the initial distribution?
CL: The frontline health care workers are priority A1 as well as are our elderly who are in care facilities. So it makes sense for the majority of it to be distributed it hospitals.
The down side of this people are exhausted. They have been working overtime. The hospitals are reaching capacity. So it’s really hard to put this burden on them right now.
SN: It sounds like these are reversible problems as more distribution sites are identified and as more sites are identified.
CL: I think, yes. I hope we can fix some of these issues that are limiting distribution and we can get these things out faster. At the current rate we’re going it’s going to be four years before we immunize all New Yorkers. So we clearly have to have a better mechanism.
I think one of the things that could have been done which I am disappointed wasn’t was we had 10 months to be ready to distribute this vaccine as quickly as possible. It seems like the necessary preparation steps weren’t done and all the consideration before we tried to roll this vaccine out.
SN: What could have been done sooner in order to get to a better place?
CL: We have a lot of technology that we can take advantage of and I feel like a lot of this is being done old school. The communication between distribution sites has been pretty smooth although I disagree with fining distribution sites if they don’t move too quickly.
I think what we could have done is develop a better platform — I don’t know if that would have been nationwide or state by state — to try and organize the distribution more effectively.
I witnessed photos of our older population in Florida sitting in lawn chairs in huge lines waiting to get the vaccine. This shouldn’t be happening. We can be better organized with our technology today.
SN: Are we seeing these issues unique to our state or are they all over the country?
CL: I think we’re seeing this everywhere. Some of the things we are encountering in New York City for example are things that we will be encountering in all the major cities. So one of the things we could do is have better communication among the individuals in charge of major distribution in all those major cities so they can see the issues coming or find solutions that are working in one place to avoid reinventing the wheel.
SN: Should local governments and county public health play an expanded role?
CL: I’m torn with this issue because on the ground the local people are most informed about what’s going to work best. But the more fractured we get and the more different people who are in charge of this in different places just creates more confusion and makes it more difficult to communicate.
Yes, we need to involve them. Should they be in charge of it? I’m not sure. I think we need a hierarchy of communication. The number one thing is everyone is on board, everyone is working together and we’re trying to get this vaccine out as quickly as possible.